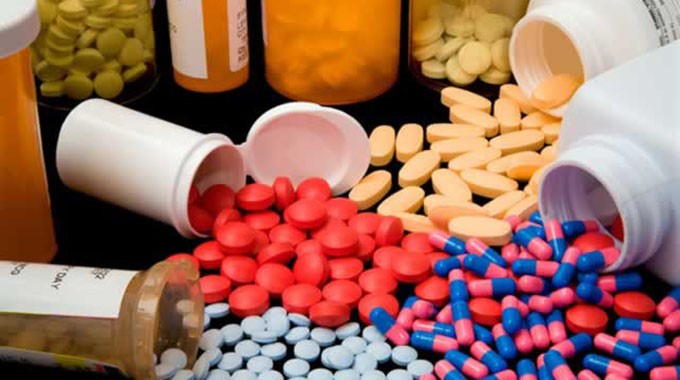
When one has malaria-related symptoms, they are likely to rush into a chemist and get the right antibiotics in order to treat it before a necessity to visit hospitals. One may get the medicine and it may fail to treat the symptoms and in some instances accelerate the illness. This may be attributed to the counterfeit medicines making their way into Kenya and Africa as a whole. This slows the achievement of sustainable development goals in the health sector.
As most people tend to curb the unemployment rate, they venture into easy money making ways. This has led to an increase in quack clinics and briefcase pharmacies and chemists. Most of these clinics and pharmacies operate illegally in Kenya’s private sector making it hard to ascertain the standard and non-standard. Selling of counterfeit medicine by these clinics has been a problem for most governments in Africa. This has raised concerns by experts in the health sector as thousands of people die as a result of consuming these non-standard drugs.
The counterfeit drugs are said to have the wrong ingredient sizes and at times no ingredients at all related to treating the disease they are intended to. This poses danger to individuals and at times can cause deaths of patients.
Kenya malaria indicator survey conducted a survey in 2015 that indicated that about twenty-five percent of children attend private health care facilities in relation to malaria treatment. These children are most threatened by the ailment due to weak immune systems. In urban areas, the figure was shown to be at forty percent. The issuance of malaria medicines such as artemisinin combination therapies (ACTs) is said to exist in a large number in private sectors. These medicines lack international and local approval.

Figure 2image source: capitalfm.co.ke
In 2014, the pharmacy and poisons board (PPB) conducted thorough surveillance that saw the closure of many illegal pharmaceutical shops around Kenya. Suspects totaling up to 926 were arraigned in court regarding this issue.
However, in 2017 the malaria journal published a study in line with the malaria treatment medicines. In the study, it was still found that artemisinin combination therapies were still thriving in the private sector. Approval from world health organization (who) and the global fund to give a subscription of the medicine was not given at the time. In fact, its popularity had risen from twenty-one percent to forty-one percent. Kenya has made a progressive step in incorporating technology to control the increase of fake drugs due to concerns in the health sector.

Figure 3image source: businessinsider.com.au
A majority of medicines that are used in Kenya are either from Japan or India. Opportunistic medical practitioners and those operating chemists take advantage of medicine shortage to introduce fake drugs. The government has however teamed up with pharmacy and poisons board (PPB) to include technological innovations that will see the end of fake drugs.
A spectrometer has been introduced as a technological device to reduce the spread of counterfeit medicine. This is a tiny portable device with the ability to scan medicine ingredients. It scans the active ingredients and if none is found it issues an alert making it easy to differentiate between the standard and non-standard drugs.
Mobile use in Kenya has increased over time. A majority of the present population has access to mobile phones as compared to a decade ago. Pharmacy and poisons board has come up with mobile-based innovations that will see people have the ability to identify genuine and fake drugs. This is through the creation of a code that is accessible to people at chemists and will aid in identifying the quality of medicines. In addition to this, the code scans through and identifies various side effects caused by various medicines and if medicines are registered or not. Online licensing of drugs and pharmaceutical shops have also been incorporated in order to meet the standards centered on drugs that make their way into hospitals and chemists.
Regardless of incorporating the use of technology to identify the counterfeits, the main problem remains untapped. Health care in Kenya if faced with a lot of problems which should be solved before tackling the big problems. There is limited access to health care facilities. This leads to the increase in the purchase of over the counter drugs which in most cases are not genuine.
The lack of adequate personnel in hospitals also leads to an increase in the rise of counterfeit drugs. imagine going to a hospital and finding a long queue at the consultation room waiting for one doctor to treat all patients. This would prompt to seek fast services at a pharmaceutical clinic especially when one can attribute the symptoms to a particular illness. Health care financing is also low and most public hospitals, for instance, prescribe medicines that one has to look for elsewhere. This leads to searching the drug in a chemist and without the knowledge of identifying a fake or genuine drug one ends up purchasing as most share similar names.
Despite the government finding a solution to ending counterfeit medicines, the problems seem to resurface in a unique way as time goes by. It is wise to solve the problem from the root. Once a farmer notices a problem with a crop he diagnoses the root, not the branch. Diagnosis of the problem in counterfeit drugs without the health sector as a whole will lead to temporal solutions that are not beneficial in the long run.